Fungal Infections: Types of Infection
Types of Infection
Antigen Alert
It is often difficult to diagnose systemic fungal infections. Many times they are confirmed only at autopsy. Because so many systemic fungal infections go undetected and untreated, antifungal therapy has mixed success.
There are a number of different types of infections caused by fungi, including …
- Superficial infections These fungal infections affect the skin or mucous membranes. Superficial fungal infections (e.g., yeast vaginitis, oral thrush, and athletes foot) affect millions of people worldwide. Although rarely life-threatening, they can have debilitating effects on a person's quality of life and may in some cases spread to other people or become invasive (systemic). Most superficial fungal infections are easily diagnosed and can be treated effectively.
- Systemic infections These occur when fungi get into the bloodstream and generally cause more serious diseases. Systemic fungal infections may be caused either by an opportunistic organism that attacks a person with a weakened immune system, or by an invasive organism that is common in a specific geographic area, such as cocci and histoplasma. Unlike superficial infections, systemic fungal infections can be life-threatening.
- Opportunistic infections As previously noted, the fungi attack people with weakened immune systems. These can be either systemic or superficial infections.
Several kinds of fungal infections are described in the following sections.
Candida Infection
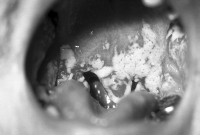
Oral thrush. (Courtesy CDC)
Candida is a yeast that is common in people—hundreds of thousands of them live peacefully in our bodies. They are found on the mucosal surfaces of the mouth, the gut, and the female reproductive system. Most Candida infections occur on one of those three surfaces. These infections can usually be treated with antifungal drugs, but drug resistance is becoming more and more common, making these infections tougher to cure. Candida can also cause more serious systemic infections.
Potent Fact
The fungi that cause infections in people are divided into three groups: yeasts, moulds, and dermatophytes. Only about 180 of the 250,000 known fungal species are able to cause disease. Most of them are moulds, but there are also many disease-causing yeasts. Some fungi are highly pathogenic and can establish a systemic infection in exposed individuals. Others only cause disease when the immune system is weak.
These infections are opportunistic and occur when the environment in the body becomes favorable for the organism to grow and spread. This can happen, for example, when someone is being treated with antibiotics. In this case, fungi, which compete for nutrients with bacteria within the body, proliferate once the bacteria are eliminated.
Yeasts in the body like Candida are usually contained through competition with other microorganisms and the action of host defense systems, such as an intact skin, salivary secretions, and antibody and cell-mediated immunity. Yet, suppression of these systems by antibiotic therapy and or by disease related immune modulation gives this organism sufficient competitive advantage so that it can dominate. This leads primarily to superficial disease but may also result in invasive fungal disease.
Potent Fact
Candida vaginitis, commonly called “yeast infection,” is a problem that 75 percent of women will experience in their lifetime. Nearly half of all college-age women will have had at least one episode of a yeast infection.
Fungal Meningitis
Fungal meningitis, an infection that causes inflammation of the membranes covering the brain and spinal cord, is one of the most common life-threatening opportunistic infections of HIV patients. It is caused by Cryptococcus, a fungus that has been found throughout the world. Infections in people are acquired by inhalation of small fungal cells spread on air currents. The organisms survive and spread only in people with weakened immune systems.
The symptoms of fungal meningitis differ from one patient to another, but can include headaches, drowsiness, and confusion. In order to differentiate fungal meningitis from bacterial and viral meningitis, blood and spinal fluid must be tested. The diagnosis is fast if fungal cells are seen in cerebrospinal fluid examined under a microscope. There is also a rapid blood test for blood and spinal fluid that gives positive results in over 90 percent of cases.
The frequency of fungal meningitis has been decreasing in the United States and Europe since the mid-1990s due to the development of more effective antiretroviral therapy for AIDS patients and preventive treatment regimens. Successful treatment of invasive disease involves various antifungal drugs, most given intravenously, but treatment failures are common due to drug resistance. In non-AIDS patients, drug therapy lasts 6 to 10 weeks. Most AIDS patients relapse within six months after treatment ends, so they are usually given lifelong maintenance treatment with an oral antifungal drug.
Antigen Alert
Beware of white statues. Pigeon droppings are a major source of Cryptococcus because the organism grows very well in the nitrogen rich excrement.
Aspergillis
Aspergillis is a mould that spreads through the air and can cause serious pulmonary and bloodstream infections in people with weakened immune systems. It is common in cancer patients, bone marrow transplant patients, and people with HIV. Early diagnosis is critical for successful treatment, although mortality is generally quite high. Aspergillis accounts for 30 percent of fungal infections among cancer patients and 10 to 25 percent in leukemia patients.
Potent Fact
Aspergillis moulds often live in air conditioning systems in hospitals. Hospitals need to have procedures in place to reduce the risk of spreading these moulds. Aspergillis can act as a powerful allergen, often resulting in Aspergillis asthma.
The disease is tough to diagnose because it often occurs in people whose immune systems are deficient, and those people don't show the usual signs and symptoms that would lead the doctor to look for a fungal infection. Also, more invasive diagnostic techniques, such as biopsies, that would be used in healthy people are more dangerous to someone with an immune system problem.
The best way to deal with Aspergillis infection is to prevent it, but that's tough because the spores are found everywhere—in the soil, the air, and the water! There are spores in your house—in the basement, bedding, air conditioning, potted plants, wicker, and dust.
PCP: Pneumocystis Pneumonia
Infectious Knowledge
PCP was one of the first unusual infections observed early in the AIDS epidemic.
PCP was one of the first unusual infections observed early in the AIDS epidemic and suggested that patients had weakened immune systems. Approximately 60 percent of people are infected with pneumocystic fungi by the time they are four years old. After a mild infection in childhood, the organism remains latent until weakened immunity triggers a reactivation. The organism lives in soil and water.
PCP has a 40-day incubation period in AIDS patients, and the disease may be accompanied by weight loss, malaise, diarrhea, dry cough, shortness of breath, and low-grade fever. In other types of patients, the onset is subtle, with an average incubation period of 60 days and resulting in a dry cough that can progress to more severe respiratory distress. Besides AIDS patients, people at highest risk for the disease include infants with severe malnutrition, children with primary immune system deficiencies, patients with cancer, and transplant patients.
Patients at highest risk for PCP also include infants with severe malnutrition, children with immune system deficiencies, and recipients of organ or bone marrow transplants. PCP is treatable, and patients at high risk for it can take preventive medicine. Early detection and treatment are the key to beating the illness.

Excerpted from The Complete Idiot's Guide to Dangerous Diseases and Epidemics © 2002 by David Perlin, Ph.D., and Ann Cohen. All rights reserved including the right of reproduction in whole or in part in any form. Used by arrangement with Alpha Books, a member of Penguin Group (USA) Inc.







