Anatomy and Physiology: Jack-of-All-Trades
Jack-of-All-Trades
The next step, and by far the most eventful one, is the three- to five-hour ride through the three parts of the small intestine (in order: duodenum, jejunum, and ileum—the last length is closest to the pelvis, which should make its location easy to remember, being so close to the ilium). The action of enzymes is intense here, as most of the digestion happens here. Some of the enzymes come from the epithelium of the small intestine itself, while the rest come from the pancreas, with bile (not an enzyme, but an emulsifier), alone, coming from the liver, via the gallbladder.
The enzymes, their origin, location of action, and the action of the enzymes themselves, are all outlined in a table further on. A primary function that has yet to be outlined is the absorption of nutrients. Since absorption occurs through the cell membrane surfaces along the lumen of the mucosa, it is crucial that that surface area be maximized. That is accomplished in part through folds in the lining called plicae, each lined with thousands of finger-like villi that make it feel like velvet. On a microscopic scale, the edge of each epithelial cell along each villus contains even smaller projections called microvilli (see Figure 14.5). The sum total of all these surfaces makes the surface area of the small intestine the size of a doubles tennis court!
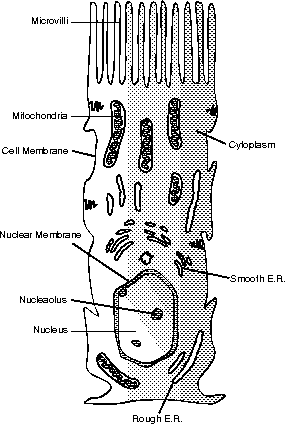
Figure 14.5
The cells of the villi increase the surface area for absorption through a “brush border” of microvilli.Once absorbed through the microvilli, the nutrients are then absorbed into the vessels in each villus. Lipids are absorbed into the lacteal, which then empties into the cisterna chyli before ultimately emptying into the blood at the left subclavian vein. All other monomers are absorbed into the capillaries and then sent directly into the liver via the hepatic portal vein, as discussed in The Respitory System. This allows excess nutrients, as well as toxins, to be processed directly by the liver.
There are some rather somber-sounding intestinal crypts at the base of the villi. There are stem cells within that constantly produce more epithelial cells to replace the intestinal mucosa. The epithelial cells last only a few days because of the constant wear and tear on the small intestine. The gastroenteric reflex stimulates peristalsis of the small intestine, whereas the gastroileal reflex causes the ileocecal valve to relax, thus stimulating movement into the large intestine, our next stop.
Trash Compactor
The large intestine (also known as the colon) is primarily concerned with the absorption of water, which is the most important step in the making of feces. The parts of the large intestine can be seen in Figure 14.6. Remember, quite a large amount of mucus is secreted into the digestive tract, both to ease peristalsis, as in the esophagus, and to protect you from digesting yourself, as in the stomach.
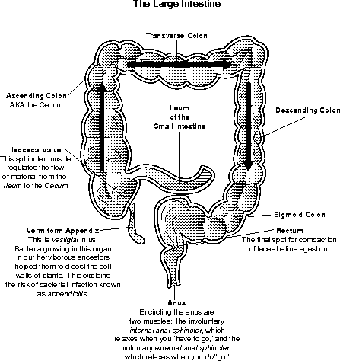
Figure 14.6The cecum, vermiform appendix, and the parts of the large intestine. (LifeART©1989-2001, Lippincott Williams & Wilkins)
If we didn't have a way of recovering some of that fluid, or at least the water portion, we would quickly dehydrate (see Figure 14.7). To give you some perspective, about 1,200 to 1,500 ml (remember, a 2-liter bottle has 2,000 ml!) enter the cecum (or start of the colon) through the sphincter known as the Ileocecal valve, but only about 150 to 200 ml of feces are expelled every day.
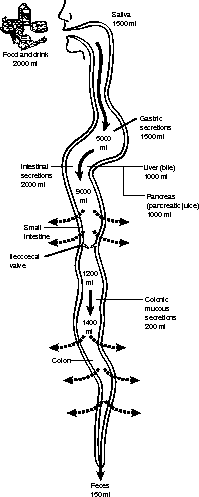
Figure 14.7The movement of fluid in and out of the digestive tract every day.
This task, however, does present the potential of some problems if the pace of the movement through the colon is not normal. The amount of time food spends in the large intestine varies from 8 to 15 hours. While it's there, a colon's gotta do what a colon's gotta do. So if the passage is too slow, and too much water is absorbed, the dehydration of the feces causes constipation. On the other hand, if the movement (pun intended, unfortunately) is too rapid, and too little water is absorbed, the person suffers diarrhea. The loss of so much water through diarrhea can result in systemic dehydration.
Flex Your Muscles
Once again, make the words work for you! Can you figure out what the “coli” in E. coli refers to? If you thought about its home, the colon, you are right!
In addition to absorbing water, the large intestine also absorbs other substances, such as vitamin K (which the liver uses to make clotting factors), biotin (for many reactions), vitamin B5 (for making steroids and neurotransmitters), urobilinogen, bile salts, and toxins (all three to be excreted by the kidneys). Pigments from the breakdown of urobilinogen are what make feces brown!
A little space needs to be made here for our companions, the bacteria known as intestinal flora. The most famous of these is Escherichia coli (E. coli to its friends). People these days have a misguided idea of bacteria. The common misconception is that all bacteria are bad; nothing could be further from the truth. Apart from the ecological impact of bacteria, especially in terms of the nitrogen cycle in soil, bacteria are necessary for our survival!
About half of our daily vitamin K needs come from intestinal bacteria and is absorbed through the walls of the colon. These bacteria also break down undigested peptides and plant matter in the feces, thus producing a medley of gases, including hydrogen sulfide (H2S), known as flatus (which is why farting is known in kinder circles as flatulence). So, next time you, shall we say, “break wind,” it's not your fault; blame it on bacteria!
The End of the Tunnel
The final resting place for the compacted feces is in the last 6 inches (15 cm) known as the rectum. One interesting thing to note about the rectum is the pair of sphincter muscles that surround the anal opening. Without knowing about their existence, we have all experienced the effects of each of these sphincters. As I stated in The Muscles, given that all muscles contract, a circular sphincter muscle will close the aperture when contracted, and the aperture will open when the muscle relaxes.
That being said, let me introduce you to the internal and external anal sphincters. Perhaps what distinguishes them is their nervous control. The internal muscle is involuntary, but the external is under our voluntary control. Imagine now that it has been a long time since you have defecated, and the feces is starting to pile up and exert pressure on the stretch receptors along the rectal wall. This will trigger the relaxation of the internal anal sphincter, which will cause a great deal of pressure on the external anal sphincter. At this point the only thing standing between you and extreme social embarrassment is the contraction of that voluntary external sphincter! In essence, when the internal sphincter relaxes, you “have to go,” and when the external sphincter relaxes, you “do go”!

Excerpted from The Complete Idiot's Guide to Anatomy and Physiology © 2004 by Michael J. Vieira Lazaroff. All rights reserved including the right of reproduction in whole or in part in any form. Used by arrangement with Alpha Books, a member of Penguin Group (USA) Inc.
To order this book direct from the publisher, visit the Penguin USA website or call 1-800-253-6476. You can also purchase this book at Amazon.com and Barnes & Noble.







